This week we’re going to take a look at one of the surgical procedures that was used to treat TB and to counter some of it’s side-effects. A register of operations held within the collection lists a number of different procedures that were carried out on the patients, the majority having been performed by the visiting surgeon Mr Johnston. These procedures were employed predominantly before the advent of effective antibiotics but many of them still continued to be used effectively after the introduction of drug therapies. Over the coming months we will explore a range of different treatments that were employed at Stannington, beginning this week with tenotomy.
The records of Stannington Sanatorium show tenotomy to have been performed on several patients suffering from tuberculosis of the bones and joints. The procedure involved the division of the tendon to lengthen it and would be performed in order to counter deformity caused by the tuberculous disease and increase flexion in a particular joint. The tendon would be divided, with the two sections allowed to pull apart and then allowed to re-heal at the overlap of the two parts thus resulting in a lengthening of the tendon. This is not a procedure exclusive to the treatment of tuberculosis but rather in tackling any disease or deformity that has adversely affected the joint. Patients could find themselves unable to fully flex a particular joint and may be left holding it at an unusual angle owing to muscle contracture and possible subluxation, whereby one muscle pulls more strongly than its counterpart causing partial or complete dislocation of the joint. Following the procedure the affected joint may be put in plaster or splinted to ensure that the tendon heals at the new length and the joint is in the correct position.
Patient 83/39 was one patient that underwent the procedure, in this particular case division of the hamstrings to tackle poor flexion in the right knee. Female and aged 3, patient 83/39 was admitted to the sanatorium on 22 October 1937 with a positive mantoux test and the affected knee described as hot, swollen and having limited flexion. Her pre-admission report reads:
“Fell and after 14 days R knee began to swell and began to limp. Went to Durham County Hosp. & leg was immobilised in plaster 4 times. Typical tub. R knee joint probably synovial type.”
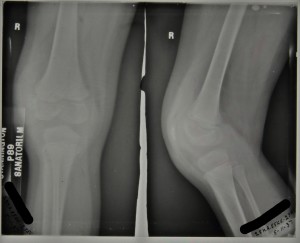
The above radiograph was taken in November 1937, two weeks after admission, with the x-ray report as follows ‘Thickening of capsule. Eburnation and erosion of femoral condyles, especially outer.’
Her progress is noted in her file throughout her stay and in May 1938 it is reported that the flexion in her knee is at 45 degrees and in August 1938 it is decided that she should have her hamstrings divided with the procedure carried out by Mr Johnston on 17 August 1938. There appears to be some initial progress as in September 1938 flexion in the right knee is now reported to be 50 degrees and by October she was wearing a Thomas splint (a traction splint commonly used to immobilise the leg).
During 1939 progress appeared to be limited with flexion remaining at around 45 degrees throughout, but by January 1940 we see reports that the knee has improved and is almost straight. In April 1940 she was walking well and she was eventually discharged on 9th August 1940 able to walk in a splint. It is debateable as to how much impact the division of the hamstrings had on the eventual straightening of the knee and how much was down to the long term splinting and immobilisation of the joint but she was nonetheless eventually discharged as quiescent. The two radiographs below were taken later on in her stay and date from c.1939/40,
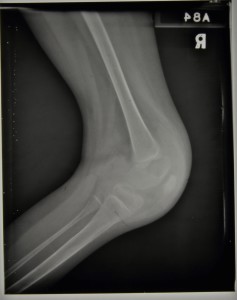
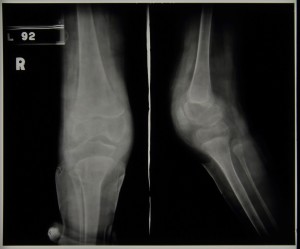
Sources:
J. Krol, Surgery for Deformities Due to Poliomyelitis, (Geneva: World Health Organisation, 1993)